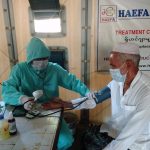
Health workers on the ground in the overcrowded refugee camps in Cox’s Bazar, Bangladesh, where an estimated 855,000 Rohingya refugees currently reside, have been waiting anxiously for weeks for their turn to come.
On June 2, the news finally broke: the first death from COVID-19 was recorded in the refugee camps and at least 29 other refugees have tested positive for the coronavirus.
Now that this grim milestone has been reached, it is up to the many international and national organizations providing essential care and services in the camps to address this looming crisis, as they change priorities and shift already limited resources to mitigate the risks associated with coronavirus and to ensure effective response. Myriad challenges exist, but central to these groups’ shared mission is how to maintain humanitarian assistance, such as health care and food provision, while doing what they can to halt the transmission of the virus.
Public Health Challenges
The Rohingya fled widespread and systematic violence in their communities in Myanmar in August 2017, and are now residents in the world’s largest refugee settlement.
Cramped living conditions in the camps make it impossible to practice physical distancing to prevent the spread of the coronavirus or to self-isolate if infected, as advised by the World Health Organization. Health infrastructure in the camps is not able to meet the demands of the current non-COVID-19 caseload and is therefore not likely to have the capacity to respond to additional pressures if and when an outbreak of COVID-19 occurs. There are currently only five hospitals across the collection of 34 camps housing nearly a million people, though humanitarian organizations have been working to quickly build isolation and treatment centers.
One such organization is Health and Education for All (HAEFA). HAEFA runs two health centers in Kutupalong and Balukhali camps, which, before the COVID-19 pandemic, provided medical care to between 6,000 and 7,000 patients a month.
More than one in five refugees is at high risk for developing severe complications if infected with the coronavirus.
HAEFA President Dr. Ruhul Abid, associate professor at Brown University Alpert Medical School and at Rhode Island Hospital, believes that, in addition to continuing to provide care to patients, HAEFA must support prevention in the community to protect the most vulnerable from the spread of the coronavirus: “The main protective mechanisms people can use against COVID-19 are social distancing and hygiene. In a place like [the] Rohingya camps, this is not possible. HAEFA is planning to provide cloth masks, bar soaps, toilet brushes, bleach, and household hand-washing stations to our elderly patients with comorbidities such as hypertension, diabetes, asthma, and tuberculosis. They are most vulnerable and may have severe outcomes if infected with COVID-19. It is our responsibility to help them protect themselves,” he said.

An average of 150 patients per day are still coming to HAEFA clinics for a variety of routine services but its staff must now enforce physical distancing in patient waiting areas and during examinations. Staff are urging patients to use the new hand-washing stations built outside the health centers.
The implementation of recommended public health measures to prevent the spread of the coronavirus is not without its challenges. Spaces are very limited, and health literacy is generally low. Dr. Ataul Labib, a medical officer at Kutupalong Medical Center, told PHR: “We have to work very carefully here. The patient has to be seen [while] maintaining distance. Everyone is using PPE [personal protective equipment] when seeing patients. Everyone washes their hands repeatedly after examining each patient. We didn’t have to do this before COVID-19.” The imperative for HAEFA staff to implement and enforce these practices is pressing, as the organization estimates that more than one in five refugees is at high risk for developing severe complications if infected with the coronavirus.

Essential Care Is Still Essential
Despite the changes to patient care practices at HAEFA health centers, patients are still seeking care for diabetes and hypertension, in addition to acute illnesses not related to coronavirus. Jannataul Mawa, a medical assistant at Balukhali Medical Center, noted that because of a lockdown and restrictions on all but essential services in the camps put in place by the government of Bangladesh, many of their regular patients stopped seeking treatment for chronic illnesses, which risks exacerbating these conditions and impacting their overall health.

This is particularly concerning because the Rohingya have experienced decades of systemic discrimination in Myanmar, long before they were forced to flee into Bangladesh. Some members of the Rohingya community had never been under a physician’s care before arriving in Bangladesh.
This lack of access – resulting in untreated, underlying health conditions and complications – increases the population’s vulnerability to coronavirus. Other health concerns will not pause because of the coronavirus pandemic and deferring treatment could increase mortality from other diseases that go untreated in addition to coronavirus. For these reasons, every effort should be made to ensure that essential and routine care can continue, despite the pandemic.
Communication Is Key
The health system within the Cox’s Bazar refugee camps relies on coordination between organizations and an active referral system to send patients to the health centers best equipped to address specific issues, whether they be mental health, surgery, or maternal health. To achieve an effective coronavirus response, these systems are even more critical. Communication restrictions put in place by the government of Bangladesh since September 2019 have severely limited the flow of information and internet access in the camps. Not only do these restrictions prevent the Rohingya communities’ access to accurate information on health services and the prevention of coronavirus, they severely hamper the ability of the camps’ health system, already a patchwork of health centers run by many different organizations, to coordinate responses and referrals effectively.

Supporting and Protecting the Caregivers
As the COVID-19 pandemic continues, organizations like HAEFA are also consumed with thinking about the safety of their staff. In the short term, HAEFA staff say they need PPE in order to provide clinical care. Since March 2020, HAEFA has focused on ensuring adequate PPE is available for health care workers and is implementing a training program for 3,000 health care workers on how to treat COVID-19 efficiently and protect themselves. To that end, HAEFA recently helped organize a training-of-trainers with Project HOPE and Brown University’s Watson Institute and Center of Human Rights for health care professionals in Bangladesh.
Now that coronavirus has entered the refugee camps in Cox’s Bazar, frontline health workers like those at HAEFA must rely on protective tools, effective communication, and continuation of essential care as their first line of defense against a pandemic whose reach into this community is still unknown and whose effects could be catastrophic.
Read more about HAEFA on their website.