After George Floyd’s killing, captured on video and shown widely across the United States and around the world, millions of people took to the streets nationwide to support the Black Lives Matter movement and demand police accountability.
While protests in the United States in June and July of 2020 were overwhelmingly peaceful and without incident, some devolved into violent confrontations between police and protestors, including widespread law enforcement use of crowd-control weapons (also known as “less-lethal” weapons).
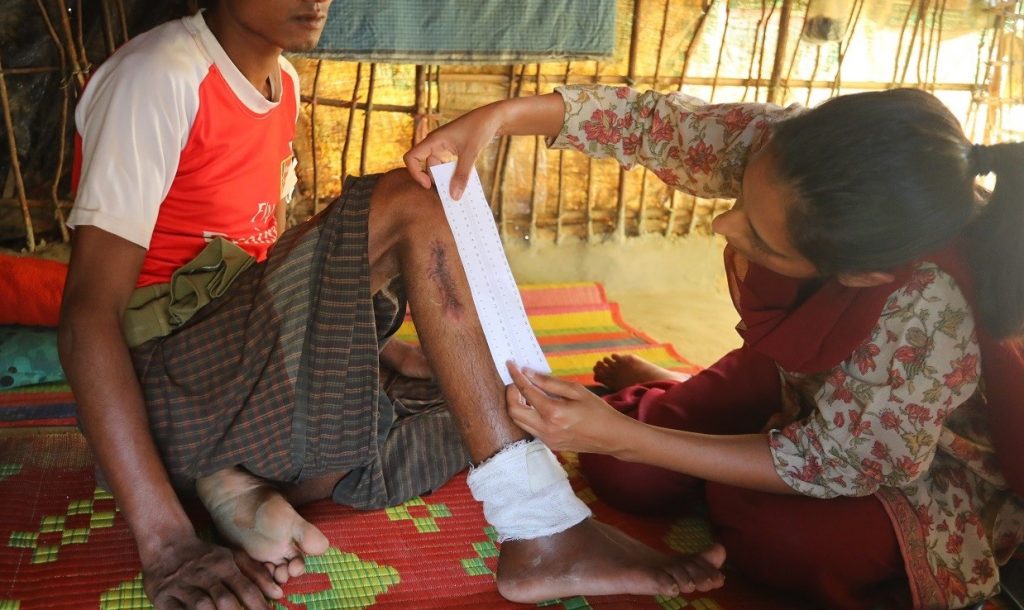
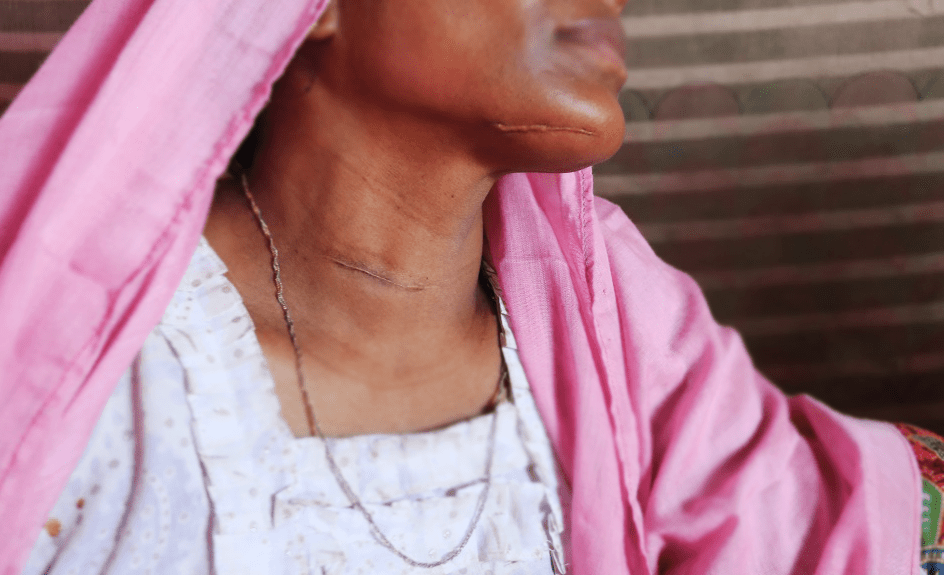
Tear gas, pepper spray, stun grenades, and acoustic weapons have all been extensively employed, but the scale of the use of kinetic impact projectiles (KIPs) stands out in reports from protestors, journalists, and bystanders. KIPs include various bullets and baton rounds, as well as tear gas canisters, that are fired into crowds from a gun, rifle, or other launcher.
In an effort to record the scope of KIP use and the resulting injuries, Physicians for Human Rights (PHR) used open-source research methods to collect publicly available data. We identified at least 115 people across the United States who were shot in the head or neck with KIPs from May 26 to July 27, 2020. Explore the presentation built on ArcGIS Storymaps below: