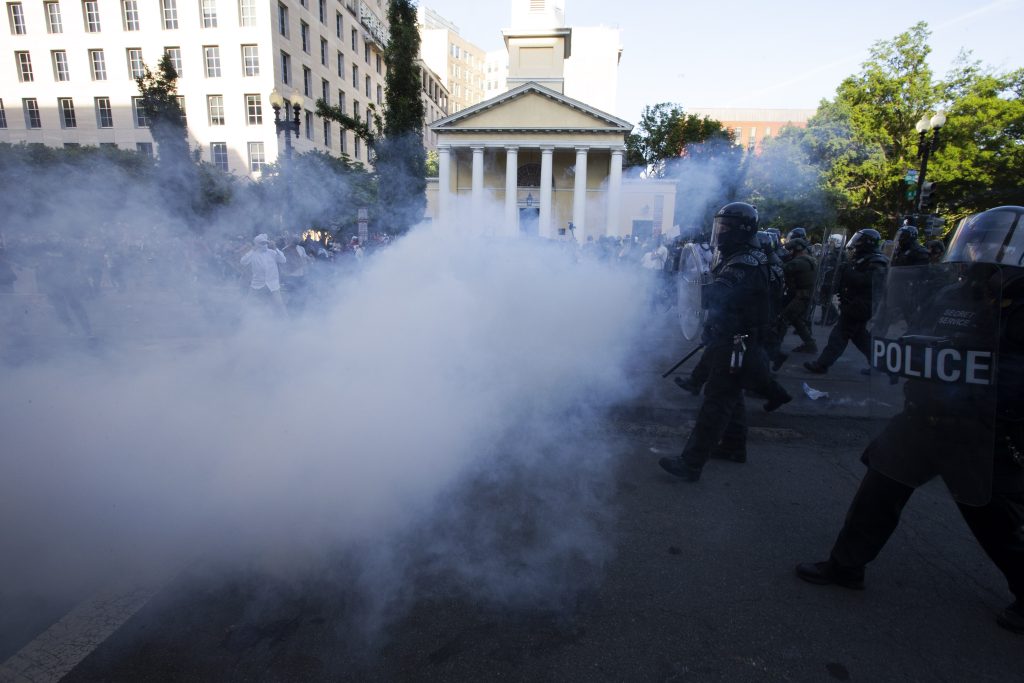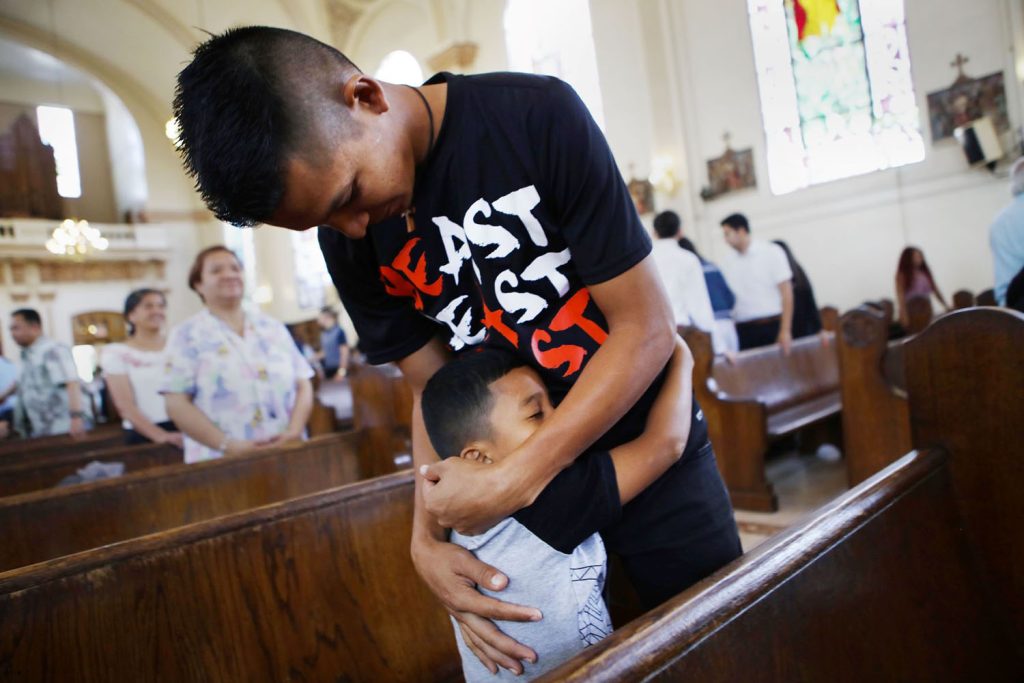The Safeguarding Health in Conflict Coalition (SHCC), of which PHR is a part, has released a report (available in English and Ukrainian) documenting 394 incidents of violence against or obstruction of health care in Ukraine in 2023. The ongoing conflict, initiated by Russia’s full-scale invasion in February 2022, has left nearly a fifth of Ukraine’s territory under occupation and has caused extensive damage to civilian and energy infrastructure. Over 12 million Ukrainians have faced energy disruptions, and severe flooding in June 2023 further exacerbated the humanitarian crisis, affecting over sixty thousand people. About 40% of the Ukrainian population is estimated to require humanitarian assistance in 2024. Read more in the SHCC Press Release
Downloads
About
The Safeguarding Health in Conflict Coalition is a group of more than 40 organisations, including PHR, working to protect health workers and services threatened by war and civil unrest. It has raised awareness of global attacks on health and pressed United Nations agencies for greater global action to protect the security of health care. The SHCC monitors attacks, strengthens universal norms of respect for the right to health, and demands accountability for perpetrators.